Prostaglandin Analogs in Ophthalmology: Advancing Glaucoma Treatment
Comprehensive exploration of prostaglandin analogs' role in treating glaucoma, from mechanism of action to clinical applications.
In the landscape of modern ophthalmology, prostaglandin analogs have established a significant clinical profile. Over the past three decades, these compounds have advanced how the medical community approaches glaucoma management, offering documented efficacy combined with once-daily dosing regimens.
The IOP-Lowering Mechanism
The primary challenge in glaucoma management is reducing intraocular pressure (IOP) to prevent optic nerve damage. Before the advent of prostaglandin analogs, treatment options primarily focused on reducing aqueous humor production (beta-blockers, carbonic anhydrase inhibitors) or mechanically opening the trabecular meshwork (miotics).
Prostaglandin analogs introduced a novel and highly effective mechanism: enhancing the uveoscleral outflow pathway.
Uveoscleral Outflow Enhancement
The primary mechanism centers on uveoscleral outflow enhancement. This improvement results from comprehensive remodeling of the ciliary muscle architecture, where previously dense collagen bundles become progressively loosened, creating expanded extracellular spaces that facilitate fluid movement. The aqueous humor gains easier passage from the anterior chamber, flowing posteriorly through newly widened intermuscular channels, accumulating in the suprachoroidal space, and ultimately exiting through the sclera or entering the episcleral venous system.
Research utilizing advanced imaging techniques has confirmed that this is not merely a functional change but a structural one. Matrix metalloproteinases (MMPs) are upregulated, leading to the remodeling of the extracellular matrix within the ciliary body. This explains why the IOP-lowering effect of prostaglandin analogs can persist even after a dose is missed—the structural changes facilitate sustained outflow.
Evolution of the Molecule
The development of commercial prostaglandin analogs required overcoming significant chemical challenges. Natural prostaglandins are rapidly metabolized and can cause significant irritation. The breakthrough came with the modification of the prostaglandin F2α molecule.
Latanoprost: The First Generation
Latanoprost represented the first commercially successful prostaglandin analog for glaucoma. By esterifying the carboxylic acid group, researchers improved corneal penetration while minimizing irritation. Once inside the eye, corneal esterases hydrolyze the prodrug into its active acid form, which then targets the FP receptors in the ciliary body.
Bimatoprost and Travoprost
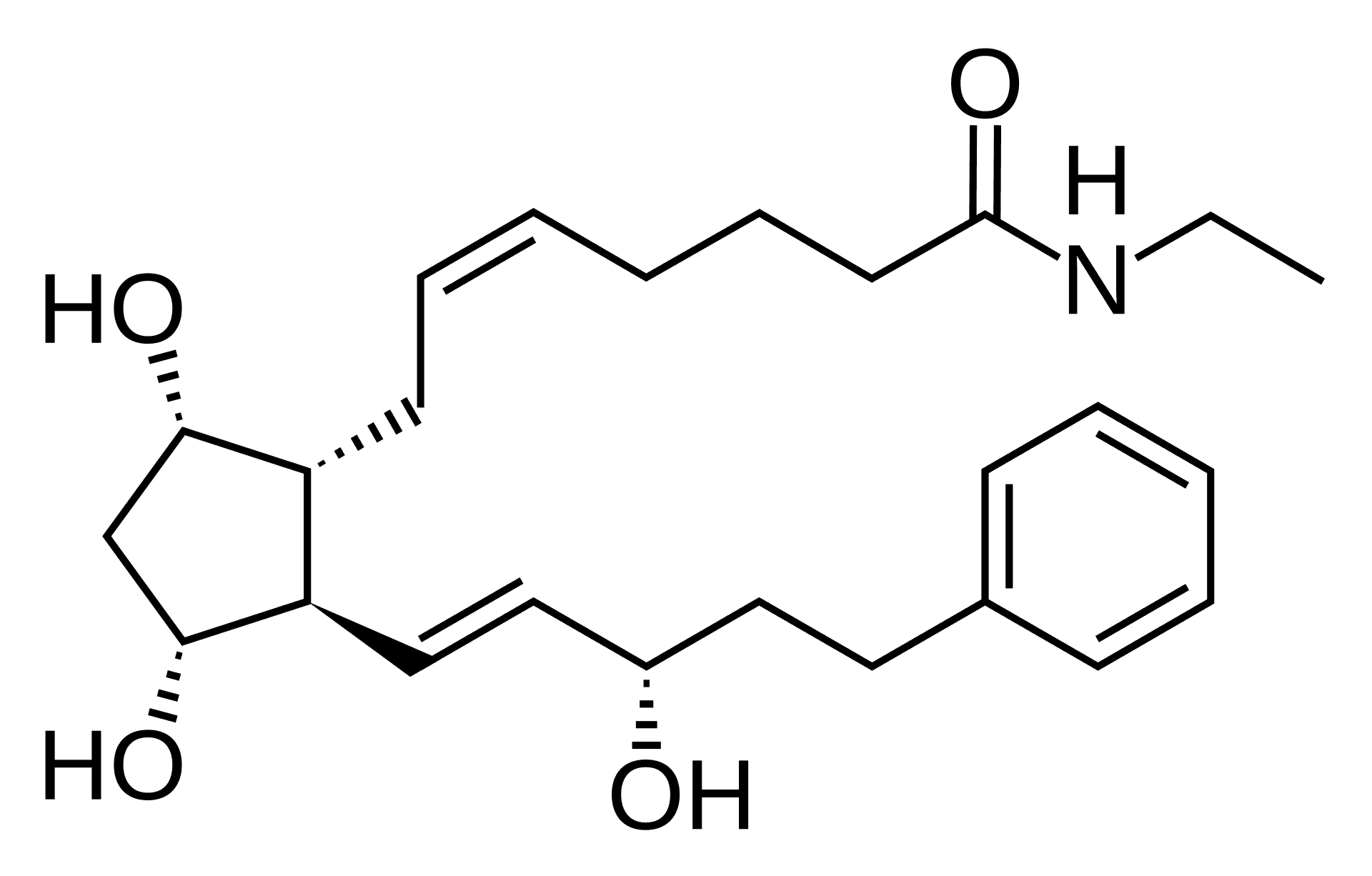
Subsequent developments led to bimatoprost and travoprost. Bimatoprost is unique as it is a prostamide—structurally similar to prostaglandins but with an amide group replacing the ester. This structural difference alters its receptor binding profile and metabolic pathway.
FDA approval came in 2001, and bimatoprost quickly established itself as a potent option in the prostaglandin class. Long-term efficacy studies confirm that bimatoprost's therapeutic effect persists over years of continuous use without tachyphylaxis.
Clinical Efficacy and Safety Profile
In head-to-head clinical trials, prostaglandin analogs have consistently demonstrated superior IOP lowering compared to beta-blockers, the previous gold standard. A meta-analysis of randomized clinical trials showed that prostaglandin analogs typically achieve IOP reductions of 30-35% from baseline, compared to 20-25% for beta-blockers.
Systemic Safety
One of the most significant advantages of this class is the lack of systemic side effects. Unlike beta-blockers, which can cause bradycardia, bronchospasm, and fatigue, prostaglandin analogs have a safety profile primarily limited to local ocular effects. This makes them particularly suitable for elderly patients with comorbid cardiovascular or respiratory conditions.
Future Directions
The success of prostaglandin analogs has spurred continued research into optimizing their delivery and efficacy.
Preservative-Free Formulations
Chronic exposure to benzalkonium chloride (BAK), the most common preservative in eye drops, can lead to ocular surface disease. New formulations using alternative preservatives or single-use preservative-free vials represent a significant advancement for patient comfort and compliance.
Sustained Delivery Systems
The next frontier lies in removing the burden of daily adherence. Intracameral implants releasing bimatoprost over several months are currently in advanced clinical stages. These sustained-release systems ensure 24/7 therapeutic coverage and eliminate the variability of patient compliance.
Conclusion
Prostaglandin analogs remain the cornerstone of medical glaucoma therapy. Their unique mechanism of action, utilizing the eye's natural drainage pathways, combined with a robust safety profile, ensures their continued dominance in the ophthalmic pharmacopeia. As delivery systems evolve, the utility of these versatile molecules will likely extend well into the future, preserving vision for millions of patients worldwide.